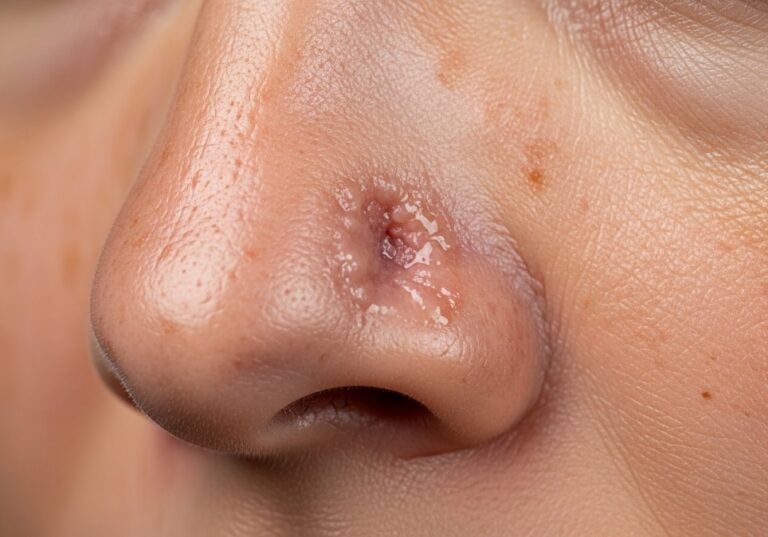
Basal cell carcinoma stands as one of the most prevalent forms of skin cancer worldwide, affecting millions each year. This condition originates in the basal cells, which reside in the deepest layer of the epidermis, the skin’s outermost barrier. These cells are responsible for regenerating new skin as older layers shed naturally. When mutations occur in their DNA, uncontrolled growth ensues, leading to the formation of cancerous lesions. Although it progresses slowly and seldom spreads to distant parts of the body, timely intervention is crucial to prevent local tissue damage and potential disfigurement.
The disease primarily manifests on areas frequently exposed to sunlight, such as the face, neck, and arms, but it can appear anywhere on the body. Its insidious nature means that many individuals overlook early signs, mistaking them for benign skin changes. However, with rising awareness and advancements in dermatological care, detection rates have improved, contributing to high cure rates when addressed promptly. Health organizations emphasize the role of ultraviolet radiation as a key culprit, underscoring the need for protective measures in daily routines.
Understanding this cancer involves recognizing its multifaceted impact on health. From cosmetic concerns to rare but serious complications, it affects quality of life in various ways. Public health campaigns highlight its preventability, encouraging regular skin examinations and lifestyle adjustments. As research evolves, new insights into genetic predispositions and environmental triggers continue to shape prevention and management approaches.
Global statistics reveal a steady increase in diagnoses, attributed to longer lifespans and greater outdoor activities. In regions with intense sunlight, incidence rates soar, affecting diverse populations. Medical professionals advocate for education on self-monitoring, as early lesions are often asymptomatic yet treatable with minimal intervention.
Symptoms and Early Signs
The initial presentation of basal cell carcinoma can be subtle, often resembling non-cancerous skin conditions. Common indicators include persistent skin changes that do not resolve over time. These alterations may start small but gradually enlarge, prompting individuals to seek evaluation. Vigilance is key, as the cancer’s slow growth allows for early intervention before significant progression.
Lesions typically appear as raised or flat areas with distinct features. They might develop a crust or scab that repeatedly forms and falls off, leading to intermittent bleeding. In some cases, the affected area feels itchy or tender, though pain is not always present. Monitoring for these changes, especially on sun-prone regions, is essential for early detection.
Different morphological types exist, each with unique characteristics. Nodular forms are the most frequent, presenting as dome-shaped growths. Superficial variants spread horizontally, while infiltrative types burrow deeper, making them more challenging to treat. Recognizing these variations aids in prompt medical consultation.
Common Appearances
- A shiny, translucent bump that may appear pearly or waxy, often with visible tiny blood vessels running through it. This nodule can bleed easily and form a scab that heals temporarily but recurs. On lighter skin tones, it tends to be pink or flesh-colored, while on darker skin, it might present as brown or black, mimicking a mole.
- A reddish or irritated patch that feels rough or scaly to the touch, sometimes with a raised border. This area may crust over, itch persistently, or cause a burning sensation. It often expands slowly over months, affecting larger sections of skin if left unchecked, and can be mistaken for eczema or psoriasis initially.
- An open sore that refuses to heal, oozing clear fluid or blood intermittently. The wound might scab repeatedly but break open again with minimal trauma. Surrounding skin can become inflamed, and the sore’s edges may appear rolled or elevated, indicating underlying cellular changes that require biopsy for confirmation.
- A scar-like area that is white, yellow, or waxy, with poorly defined borders. This lesion feels firm and may pull at the surrounding skin, creating a taut appearance. It develops without prior injury, distinguishing it from typical scars, and can gradually enlarge, affecting facial expressions or movement in sensitive areas.
- A pigmented spot with dark flecks or an irregular shape, resembling melanoma but growing more slowly. The color variation can include shades of brown, black, or blue, and it might have a shiny surface. This type is more common in individuals with medium to dark skin tones, where pigmentation masks early detection.
- A flat, flesh-colored lesion that resembles a persistent pimple or bump. It may not change color dramatically but grows steadily, sometimes developing a central depression. Touching it can cause minor bleeding, and it often appears on the trunk or limbs, areas less frequently examined during routine checks.
- A cluster of small, shiny bumps that merge over time, forming a larger growth. These can have a central indentation, giving a crater-like appearance. The surface might ulcerate, leading to discomfort during daily activities, and they commonly occur on the nose or ears, where sun exposure is constant.
- An area of skin that becomes numb or tingly, signaling possible nerve involvement in advanced cases. This sensory change accompanies deeper growth, where the cancer invades underlying tissues. Accompanying symptoms include persistent pain or a pins-and-needles sensation, warranting immediate medical attention.
These manifestations vary by individual factors such as age and skin type. Younger people might notice faster changes, while older adults see slower progression. Environmental influences, like ongoing sun exposure, can exacerbate symptoms, making lesions more prominent.
Photographs and descriptions from medical resources illustrate these signs, helping individuals identify potential issues. Dermatologists recommend monthly self-exams using mirrors to inspect hard-to-see areas. Any persistent abnormality should prompt a professional evaluation to rule out malignancy.
Causes and Underlying Mechanisms
The development of basal cell carcinoma stems from genetic alterations in skin cells triggered by external factors. DNA damage accumulates over time, disrupting normal cell cycles and leading to tumor formation. This process highlights the interplay between environmental exposures and cellular biology.
Ultraviolet radiation plays a pivotal role, causing mutations in key genes that regulate cell growth. Chronic exposure leads to cumulative harm, with certain wavelengths proving more damaging. Beyond sunlight, artificial sources contribute similarly, emphasizing the need for broad-spectrum protection.
Genetic predispositions amplify susceptibility, with inherited syndromes accelerating onset. Mutations in pathways like hedgehog signaling are common, driving uncontrolled proliferation. Research continues to uncover additional molecular targets for intervention.
Immune system function influences progression, as suppressed immunity allows tumors to evade detection. This explains higher rates in certain populations, such as organ transplant recipients. Lifestyle factors, including diet and smoking, may indirectly affect risk, though evidence is mixed.
Risk Factors
Identifying risk factors enables targeted prevention efforts. Demographic and behavioral elements combine to elevate likelihood, with some modifiable through lifestyle changes. Awareness empowers individuals to mitigate threats effectively.
Age advances susceptibility, as cumulative damage manifests later in life. However, trends show increasing diagnoses in younger groups due to recreational habits. Gender differences exist, with men often facing higher exposure through occupations.
Skin characteristics determine vulnerability, with lighter phenotypes at greater peril. Geographic location matters, as equatorial regions report elevated cases. Personal history of skin issues compounds future risks.
Key Risk Elements
- Prolonged exposure to ultraviolet radiation from the sun or artificial sources like tanning beds. This cumulative damage alters cellular DNA, particularly in childhood or adolescence, setting the stage for later development. Individuals in sunny climates or high-altitude areas face amplified threats due to intensified rays.
- Fair skin, light-colored eyes, and blonde or red hair, which offer less natural protection against UV damage. These traits result in easier sunburns and freckling, indicators of heightened sensitivity. People with these features require stricter protective measures to offset inherent vulnerabilities.
- A history of severe sunburns, especially blistering ones during youth. Such episodes cause lasting DNA harm, increasing long-term odds. Even occasional intense exposures can contribute, underscoring the importance of consistent shielding from an early age.
- Weakened immune systems from conditions like HIV or medications post-transplant. Suppression impairs the body’s ability to repair damaged cells or eliminate early tumors. This group experiences more aggressive forms and higher recurrence, necessitating vigilant monitoring.
- Family or personal history of skin cancer, suggesting genetic predispositions. Inherited mutations in repair genes elevate baseline risk. Those with prior diagnoses must adopt rigorous surveillance protocols to catch new lesions promptly.
- Exposure to toxic substances such as arsenic in water or occupational settings. Chronic ingestion leads to systemic effects, manifesting in skin changes. Historical use in pesticides heightens concern for certain populations, prompting environmental assessments.
- Radiation therapy for other conditions, like acne in adolescence. Ionizing radiation induces mutations similar to UV, with effects appearing decades later. Patients with such histories benefit from specialized dermatological follow-ups.
- Inherited genetic syndromes, such as Gorlin syndrome or xeroderma pigmentosum. These rare disorders impair DNA repair mechanisms, leading to multiple early-onset tumors. Genetic counseling and early interventions are critical for affected families.
Occupational hazards add layers of risk for outdoor workers. Protective policies in workplaces can reduce incidence. Public health initiatives target high-risk groups with education and resources.
Prevention Strategies
Preventing basal cell carcinoma revolves around minimizing harmful exposures. Simple habits integrated into daily life yield significant reductions in risk. Community efforts reinforce individual actions through awareness campaigns.
Sun-smart behaviors form the cornerstone, with timing and attire playing roles. Chemical barriers enhance physical ones, creating comprehensive defense. Regular assessments catch precursors early.
Dietary and supplemental approaches show promise, though not definitive. Avoiding known carcinogens complements these efforts. Long-term commitment ensures sustained benefits.
Effective Prevention Measures
- Avoid direct sunlight during peak hours, typically between 10 a.m. and 4 p.m., when UV rays are strongest. Schedule outdoor activities for early morning or late afternoon, and use shade structures like umbrellas or trees. This reduces overall exposure without eliminating enjoyment of the outdoors.
- Apply broad-spectrum sunscreen with an SPF of 30 or higher daily, even on cloudy days. Reapply every two hours, or immediately after swimming or sweating. Cover all exposed areas, including lips, ears, and the tops of feet, to ensure uniform protection against both UVA and UVB rays.
- Wear protective clothing, such as long-sleeved shirts, pants, and wide-brimmed hats made from tightly woven fabrics. Opt for items with UPF ratings for added assurance. Sunglasses that block 99-100% of UV rays safeguard eyes and surrounding delicate skin.
- Steer clear of tanning beds and sunlamps, which emit concentrated UV radiation. These devices accelerate skin aging and cancer risk dramatically. Seek alternatives like self-tanning products for a bronzed look without the dangers.
- Perform regular skin self-examinations monthly, using mirrors to check all body areas. Look for new growths, changes in existing moles, or non-healing sores. Document findings with photos for comparison over time, and consult professionals for suspicious changes.
- Schedule annual professional skin checks with a dermatologist, especially if in a high-risk category. These exams detect subtle abnormalities early. Discuss personal risk profiles to tailor prevention plans effectively.
- Protect children from excessive sun exposure, as early damage accumulates lifelong risk. Use child-friendly sunscreens and encourage hats and rash guards. Instill sun-safety habits young to foster lifelong adherence.
- Consider vitamin supplements like nicotinamide if recommended by a healthcare provider. Emerging evidence suggests it may lower non-melanoma skin cancer recurrence. Always consult before starting to avoid interactions or overuse.
Environmental modifications, like window films, support indoor protection. Advocacy for policy changes, such as banning youth tanning, advances public health.
Diagnosis Process
Diagnosing basal cell carcinoma involves clinical evaluation and confirmatory testing. Healthcare providers gather history to contextualize findings. Physical exams reveal characteristic features guiding further steps.
Biopsy remains the gold standard, providing definitive evidence. Various techniques suit different scenarios. Imaging supports assessment in complex cases.
Staging classifies extent, informing treatment. Follow-up protocols ensure thorough management. Patient education enhances compliance.
Dermoscopy aids visualization, highlighting patterns. Laboratory analysis details subtype and aggressiveness. Multidisciplinary input optimizes outcomes.
Treatment Options
Treatment selection depends on tumor attributes and patient preferences. Goals include eradication with minimal impact. Advances offer diverse modalities.
Surgical interventions predominate for most cases. Non-surgical alternatives suit specific situations. Advanced disease requires systemic approaches.
Post-treatment care focuses on healing and monitoring. Side effects vary by method. Personalized plans maximize efficacy.
Surgical Treatments
Surgery excels in removing localized tumors. Techniques preserve function and aesthetics. Recovery times differ by procedure.
- Mohs micrographic surgery involves layer-by-layer removal with immediate microscopic examination. This ensures complete excision while sparing healthy tissue. Ideal for facial lesions or recurrent cancers, it boasts the highest cure rates and minimal scarring.
- Standard excision cuts out the tumor plus a margin of normal skin. The sample undergoes lab analysis to confirm clear borders. Suitable for trunk or limb tumors, it offers reliable outcomes with straightforward closure methods like stitches or grafts.
- Curettage and electrodesiccation scrapes the cancer then cauterizes the base. Effective for superficial, low-risk growths. Healing occurs naturally, though it may leave noticeable scars, limiting use in visible areas.
- Cryosurgery freezes the lesion with liquid nitrogen, destroying abnormal cells. Quick and office-based, it’s for small, thin tumors. Potential side effects include swelling, blistering, and pigmentation changes, with variable cure rates.
Reconstructive techniques address defects post-removal. Anesthesia ensures comfort. Follow-up assesses healing.
Non-Surgical Treatments
Alternatives avoid incisions for select patients. These target superficial or inoperable cases. Monitoring is essential.
- Topical creams like imiquimod or fluorouracil stimulate immune responses or inhibit cell growth. Applied at home over weeks, they cause localized inflammation resolving post-treatment. Best for superficial variants, with cure rates lower than surgery.
- Photodynamic therapy uses light-activated agents to kill cancer cells. A sensitizing cream precedes light exposure. Suitable for multiple small lesions, it offers cosmetic advantages but requires avoidance of sunlight temporarily.
- Radiation therapy delivers targeted beams over sessions. Reserved for surgical contraindications or elderly patients. Effective but risks long-term skin changes or secondary cancers.
- Systemic medications, such as hedgehog inhibitors like vismodegib, block growth pathways in advanced cases. Oral administration suits metastatic or locally extensive disease. Side effects include muscle spasms and taste alterations, necessitating close supervision.
Combination therapies enhance results. Clinical trials explore innovations. Patient support addresses adherence.
Prognosis and Complications
Outcomes are generally favorable with early treatment. Recurrence risks guide surveillance. Complications arise from delay or aggressiveness.
Most cases resolve without spread. Factors like size and location influence prospects. Lifelong monitoring prevents new occurrences.
Potential issues include scarring, infection, or functional impairment. Advanced tumors demand extensive intervention. Emotional impacts warrant attention.
Research improves predictions through biomarkers. Support networks aid coping. Holistic care enhances quality of life.
Living with Basal Cell Carcinoma
Post-diagnosis, adaptation involves routine adjustments. Emotional resilience builds through knowledge. Community resources provide guidance.
Scar management techniques improve appearance. Sun avoidance becomes habitual. Dietary choices support skin health.
Family involvement fosters support. Professional counseling addresses anxiety. Ongoing education empowers decision-making.
Workplace accommodations ease transitions. Travel planning incorporates protection. Long-term wellness focuses on prevention.
Advances in Research
Ongoing studies target molecular mechanisms. Novel therapies emerge from genetic insights. Immunotherapies show promise.
Prevention research refines guidelines. Epidemiology tracks trends. Collaborative efforts accelerate progress.
Patient participation in trials drives innovation. Funding supports discoveries. Future outlooks brighten with technology.
Integration of AI aids detection. Personalized medicine tailors approaches. Global initiatives standardize care.
Conclusion
Basal cell carcinoma, while common, remains highly manageable through awareness and action. Recognizing symptoms early, understanding causes, and adopting preventive measures significantly reduce its impact. Risk factors highlight vulnerable groups, urging tailored strategies. Diagnosis and diverse treatments offer effective paths to recovery, with excellent prognoses for most. Living proactively post-treatment ensures sustained health, as research promises further advancements. Prioritizing skin protection safeguards against this and other skin concerns, promoting overall well-being.