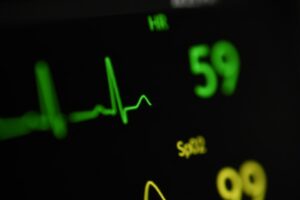
Your resting heart rate serves as a vital window into your cardiovascular health, offering immediate feedback on how efficiently your heart functions when you are not under physical stress. While many people only check their pulse during intense exercise, monitoring your heart rate at rest provides essential data regarding your overall fitness, stress levels, and potential underlying health concerns. Understanding what constitutes a normal range and recognizing when deviations require professional medical attention is a cornerstone of proactive health management.
A resting heart rate refers to the number of times your heart beats per minute while your body is completely at rest, typically after you have been sitting or lying down quietly. For most healthy adults, this number falls between 60 and 100 beats per minute (bpm). However, this range is a broad guideline rather than a rigid rule. Many factors influence this number, including your age, fitness level, emotional state, medication use, and even the time of day. Recognizing your personal baseline is more important than comparing yourself to generic averages found in textbooks.
The efficiency of your heart is often inversely related to your resting heart rate. As your cardiovascular fitness improves through regular physical activity, your heart muscle becomes stronger and more efficient at pumping blood. Consequently, it requires fewer beats to deliver the necessary oxygen and nutrients to your tissues, which often leads to a lower resting heart rate. Elite athletes, for example, frequently exhibit resting heart rates in the 40s or 50s, which is generally a sign of superior cardiovascular health rather than a medical problem.
Factors That Influence Your Resting Heart Rate
While cardiovascular fitness is a primary driver of a lower resting heart rate, your body is influenced by a complex interplay of internal and external variables. Understanding these factors can help you interpret fluctuations in your own data and decide whether a change is cause for concern or simply a normal response to your environment or lifestyle.
- Physical Activity Levels: Consistent aerobic exercise strengthens the myocardium, or heart muscle. As the heart becomes more efficient, it can pump a larger volume of blood per beat, resulting in a lower number of total beats per minute at rest.
- Stress and Emotional State: When you experience anxiety, fear, or excitement, your body activates the sympathetic nervous system, often called the fight-or-flight response. This releases adrenaline and cortisol, which directly increase your heart rate even when you are physically still.
- Sleep Quality and Recovery: Inadequate sleep, fragmented sleep, or sleep disorders like obstructive sleep apnea can place chronic strain on the cardiovascular system. When the body is deprived of proper rest, the heart rate often remains elevated to compensate for decreased oxygen levels or high cortisol.
- Medications and Supplements: Various prescription and over-the-counter substances can alter heart rhythm and rate. Beta-blockers, for instance, are commonly prescribed to lower heart rate and blood pressure, while stimulants, decongestants, and some antidepressant medications can have the opposite effect.
- Hydration and Nutrition: Dehydration reduces blood volume, forcing the heart to beat faster to maintain circulation and pressure. Similarly, high intake of stimulants like caffeine or nicotine, as well as alcohol, can act as triggers that temporarily elevate your resting heart rate.
- Underlying Health Conditions: Certain medical issues directly affect the heart’s electrical system or demand. An overactive thyroid (hyperthyroidism) speeds up metabolism and heart rate, while conditions like anemia mean the blood carries less oxygen, requiring the heart to work harder to satisfy the body’s needs.
Recognizing how these variables affect your heart rate allows for better self-monitoring. For instance, a temporary spike in your resting heart rate after a day of poor sleep, high stress, or excessive caffeine intake is often expected. However, if your heart rate remains persistently high despite managing these lifestyle factors, it may be an indication that a more thorough investigation is warranted.
How to Measure Your Resting Heart Rate Accurately
Consistency is the key to accurate monitoring. Because your heart rate fluctuates throughout the day, measuring it at the same time and under the same conditions is crucial for establishing a reliable baseline. The most effective time to measure your resting heart rate is immediately upon waking, while you are still lying in bed or sitting quietly before beginning your daily activities.
To measure your pulse manually, you can use either the radial artery on your wrist or the carotid artery on your neck. For the wrist, place your index and middle fingers gently on the inside of your wrist, just below the base of your thumb. You should feel a rhythmic thumping. Do not use your thumb, as it has its own pulse, which may confuse your count. Once you locate the pulse, count the number of beats you feel over a 30-second interval and multiply that number by two to calculate your beats per minute.
Modern technology has simplified this process significantly. Many individuals now rely on wearable fitness trackers or smartwatches that use photoplethysmography (PPG) sensors to provide continuous heart rate monitoring. While these devices are generally reliable for tracking trends, they can sometimes be influenced by device fit, skin tone, or high levels of motion. It is recommended to compare digital readings with manual checks occasionally to ensure your device’s accuracy.
What Your Heart Rate Tells You About Fitness
Your resting heart rate is one of the simplest and most accessible metrics to track your progress in a fitness program. If you have recently begun a new exercise routine, you may observe a gradual decrease in your resting heart rate over several weeks or months. This decline is a clear, measurable indicator that your aerobic capacity is improving and your heart is becoming a more efficient pump.
It is important to understand that there is a distinction between a heart rate that is low because of athletic conditioning and one that is low due to a medical condition. If your heart rate is consistently below 60 bpm and you feel energetic, healthy, and experience no symptoms like dizziness or lightheadedness, it is likely a sign of excellent fitness. However, if you are not an athlete and your heart rate is consistently low, especially if accompanied by fatigue or fainting, this condition—known as bradycardia—should be discussed with a healthcare provider.
Conversely, for individuals who have been sedentary, a resting heart rate that stays toward the upper end of the normal range (80–100 bpm) is quite common. This does not necessarily indicate a disease, but it does suggest that the heart is working harder than it needs to. Engaging in consistent, moderate-intensity cardiovascular exercise is often the most effective way to lower this number and improve long-term heart health.
When to Consult a Medical Professional
While the 60–100 bpm range covers most adults, you should not ignore persistent changes that deviate from your personal norm. It is not just the absolute number that matters, but also the stability of your heart rhythm. If you find your resting heart rate is consistently spiking above 100 bpm, a condition known as tachycardia, it is worth a conversation with your doctor to rule out underlying causes.
More importantly, you should prioritize medical attention if an irregular or fast heart rate is accompanied by specific warning signs. Symptoms that require immediate evaluation include unexplained chest pain, severe shortness of breath, persistent lightheadedness, or fainting episodes. These can be indicators of more serious electrical disturbances in the heart, such as atrial fibrillation, which can increase the risk of stroke or heart failure if left unmanaged.
When you speak to a doctor about your heart rate, providing them with a log of your measurements is incredibly helpful. Noting the date, time, your physical activity prior to the measurement, and any symptoms you felt can help your physician determine if a further diagnostic test, such as an electrocardiogram (ECG) or Holter monitor, is necessary to capture your heart’s activity over a longer period.
Pro Tips for Heart Health Management
Managing your heart health involves a holistic approach. Beyond just watching the numbers, integrating specific habits can help stabilize your heart rate and improve overall cardiovascular function. Consistency is more valuable than sporadic bursts of intense effort.
First, prioritize deep, restorative sleep. Sleep hygiene is often overlooked, but the body uses sleep to regulate hormones and lower stress levels. Creating a dark, cool, and quiet sleep environment can significantly impact your resting heart rate the following morning. Second, experiment with mindfulness and controlled breathing techniques. Practices like box breathing or guided meditation can help shift your nervous system from a sympathetic state to a parasympathetic, or ‘rest and digest,’ state, which has an immediate calming effect on the heart.
Third, keep a ‘cardiovascular journal.’ Even if you use a smart device, writing down your RHR, mood, caffeine intake, and physical activity can help you identify unique triggers. You might notice, for example, that your heart rate is consistently higher on days you consume alcohol or when you are under specific work-related stress. This insight is powerful for behavioral change.
Fourth, maintain proper hydration throughout the day. It is easy to become mildly dehydrated without feeling thirsty, yet even slight fluid deficits force the heart to beat faster. Keep water intake steady rather than relying on large amounts of fluid all at once. Finally, view your resting heart rate as a ‘diagnostic tool’ rather than a ‘performance goal.’ Do not obsess over achieving the lowest possible number, as health is multifaceted and involves many markers beyond just pulse rate.
Frequently Asked Questions
Is a resting heart rate of 95 bpm dangerous?
A resting heart rate of 95 bpm is within the normal range of 60 to 100 bpm for an adult. However, it is on the higher end. If this is your typical resting heart rate, it is usually harmless. If your resting heart rate is usually 70 bpm and it has suddenly increased to 95 bpm, you should investigate why, considering factors like stress, illness, or hydration.
Why do I feel my heart beating when I am lying down?
Feeling your heart beat, known as heart palpitations, can be caused by many factors including stress, caffeine, nicotine, or lying in a position that makes the chest wall more sensitive to the heart’s movement. In many cases, it is benign, but if it is accompanied by dizziness or chest pain, consult a physician.
Do women have a different resting heart rate than men?
Yes, on average, women tend to have a slightly higher resting heart rate than men. This can be attributed to differences in heart size and body composition. Always use your own trends over time rather than comparing your number to others.
Can I lower my resting heart rate quickly?
You cannot instantly lower your resting heart rate like flipping a switch. However, you can see temporary reductions by practicing deep breathing and relaxation. For long-term reduction, consistent aerobic exercise over several weeks is the most proven method.
Does a high resting heart rate shorten lifespan?
Some epidemiological studies have associated a higher resting heart rate within the normal range with potential health risks, but this is a complex correlation. It is more productive to focus on the modifiable factors—exercise, diet, stress management—that contribute to a healthier, more efficient heart, which naturally leads to a better heart rate profile.
Conclusion
Your resting heart rate is an incredibly useful, simple, and non-invasive metric for assessing your cardiovascular health. By understanding the normal range of 60 to 100 bpm, recognizing the factors that cause fluctuations, and knowing how to measure your pulse accurately, you can gain meaningful insights into how your body responds to lifestyle choices and environmental stressors. While a lower heart rate generally reflects better fitness, the most important aspect of monitoring is tracking your own personal baseline over time. Remember that heart health is multifaceted; while your heart rate is a critical indicator, it should be considered alongside other measures like blood pressure, cholesterol levels, and your overall sense of well-being. If you observe persistent changes, unusual rhythms, or if your heart rate is accompanied by symptoms such as dizziness or chest discomfort, seeking guidance from a medical professional is the best course of action to ensure your heart remains healthy and resilient for the long term.